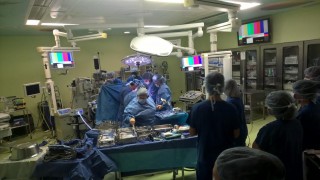
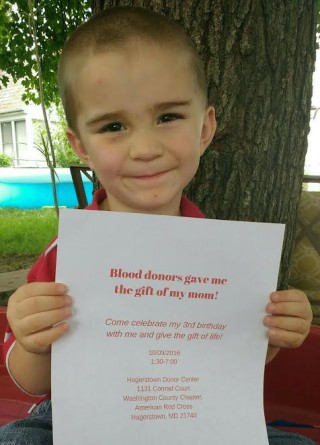
 My accreta baby is three years old. I am alive today to celebrate my baby’s third birthday because of blood donors. Even though I had very well trained and gifted surgeons, there came a point in my surgery when no matter what my surgeons did I would not have survived without blood transfusions. The human body only holds about 5 liters. I lost 7 1/2 liters of blood – my whole blood volume plus donor blood. Because of donors, I got to wake up from surgery to meet my William. I got to see my other kids grow up for the last three years. I would have missed so much if it was not for blood donors. I will never be able to personally thank those that gave an hour of their time and donated the blood that saved my life, but I can try to make sure that blood is available to others that are in need. For three years we have celebrated William’s birthday at our local Red Cross. We plan on this being a yearly event. I am beyond thankful for those that choose to donate. Blood donors are truly superheroes that save lives every day. A huge thank you to all blood donors! Please choose to be a superhero to someone today!
My accreta baby is three years old. I am alive today to celebrate my baby’s third birthday because of blood donors. Even though I had very well trained and gifted surgeons, there came a point in my surgery when no matter what my surgeons did I would not have survived without blood transfusions. The human body only holds about 5 liters. I lost 7 1/2 liters of blood – my whole blood volume plus donor blood. Because of donors, I got to wake up from surgery to meet my William. I got to see my other kids grow up for the last three years. I would have missed so much if it was not for blood donors. I will never be able to personally thank those that gave an hour of their time and donated the blood that saved my life, but I can try to make sure that blood is available to others that are in need. For three years we have celebrated William’s birthday at our local Red Cross. We plan on this being a yearly event. I am beyond thankful for those that choose to donate. Blood donors are truly superheroes that save lives every day. A huge thank you to all blood donors! Please choose to be a superhero to someone today! #ICANsavelives
#ICANsavelives
 I had my first son in October 2009. He was 10
I had my first son in October 2009. He was 10