Courtney’s Cesarean Birth Story
Early in my first pregnancy, I decided that I wanted to plan for a natural, physiologic birth. I had watched The Business of Being Born and wanted to do all in my power to avoid a cesarean section and increase the likelihood that I would be successful with breastfeeding.
My husband and I are both adopted, so my pregnancy was an extra special time for us. I became focused on researching what I needed to do to give my baby the best start to life possible.
I listened to so many podcasts and read so many books relating to birth. I frequently visited Evidence Based Birth. We found our doula. I felt prepared.
I really liked my OB. I shared my birth preferences with her and we were on the same page. However, she was just one doctor in a large practice and I knew that it was likely she wouldn’t be at the hospital when I was in labor. I underestimated, though, the impact this could have on my son’s birth.
After our hospital tour, I really considered a home birth, but my husband felt more comfortable in a medical setting, so we decided that the Birth Place at St. Joe’s was the best option for us. I had worked in acute care and felt familiar with the hospital system/setting, so I really thought we could make this work.
I felt disappointed when I tested GBS+ near the end of my pregnancy. I knew it wasn’t a huge deal, but I knew it meant they would want me to get to the hospital while I was in early labor for IV antibiotics and I had really wanted to labor at home for as long as possible to reduce the risk of unnecessary interventions. I was hoping my water wouldn’t break before labor began, as I knew that would put me “on the clock”.
My due date passed and at 40 weeks and 3 days, as I was sterilizing breast pump parts, my water broke. I called my practice and the on-call doctor recommended that I go to the hospital to start antibiotics. I took my time showering and getting the last of our things together and contractions started just as we were getting ready to leave our house.
In triage, it was confirmed that my water had broken. I consented to a cervical check, which was really rough and painful. Looking back, I think this might have been the beginning of feeling a loss of control.
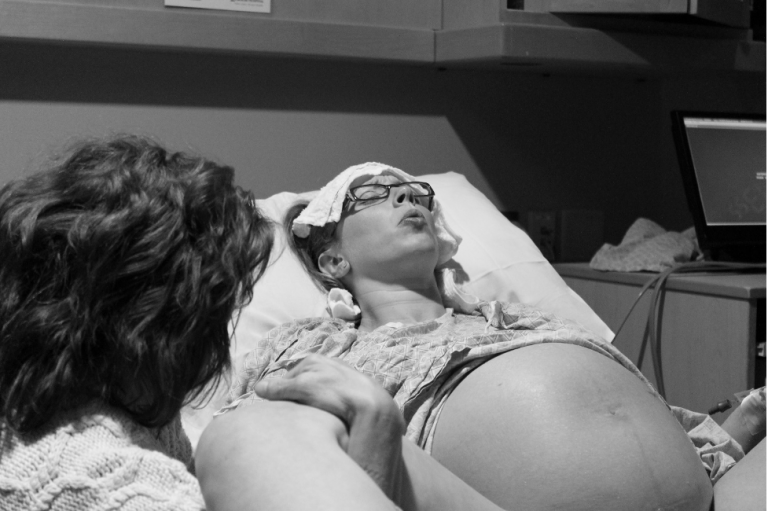
We got settled and I was able to get some sleep before waking to more intense contractions. I asked my husband to call my doula, Sarah, to have her meet us at the hospital. She was so helpful. I was able to manage contractions with help from Sarah, my husband, a hot shower, changes in positioning, and counter pressure, and after some time, I was able to get sleep between contractions.
My contractions followed an irregular pattern, so we did a lot to try to shift baby’s position. After about 12 hours, a midwife in the practice came in and recommended pitocin, expressing concern regarding an increased risk of infection. I requested more time. I remember feeling as if the midwife was thinking I was making the wrong decision. I felt I was being perceived as the “difficult patient”. I tried to push this out of my head and continue on.
18 hours after contractions started, I agreed to a cervical check. 3 centimeters and baby had only descended one station. I felt disappointed in my body and tearfully consented to pitocin.
Contractions intensified. This time is a blur. I agreed to another check at about 24 hours. 4 centimeters and baby was still high up, at the same station. To say I was discouraged is a huge understatement. I decided I needed an epidural if I was going to have enough energy to push.
I walked to the Labor and Delivery unit. It took the anesthesiologist 4 attempts to place the epidural, all while I was having some really intense contractions. I am so grateful for the nurse who let me hold her tight as I worked through those.
After the epidural was placed, I was able to sleep. Sarah and my mom left my husband and I to ourselves so that they could get some rest and we could have some time together while we let time pass.
I woke to a room full of nurses – shifting my position and asking me to help move my legs… each of which felt like they were stuck in 500 pounds of concrete. They didn’t say much directly to me. It felt like they were mostly talking to each other and occasionally at me. I was able to gather that my blood pressure dropped and baby was having decelerations.
Everything got stabilized and I fell back to sleep, waking to the same situation all over again. Matt had Sarah come back to our room.
I just remember feeling so guilty. I did this. My baby was healthy and then I decided to get an epidural for my own comfort and now my baby isn’t doing well. I was afraid for my baby’s life. I felt so much regret. And I felt that the nurses were judging me for having labored so long.
The doctor arrived to my room and was a calming presence. He explained that my baby was healthy, but labor wasn’t progressing as expected. The situation wasn’t emergent. I had time to make decisions.
I felt exhausted. And like I had no other options. After a brief discussion with my husband, I consented to a cesarean.
As they got a surgical team together, I began shivering uncontrollably and felt intense nausea. I got some zofran and then more in the OR.
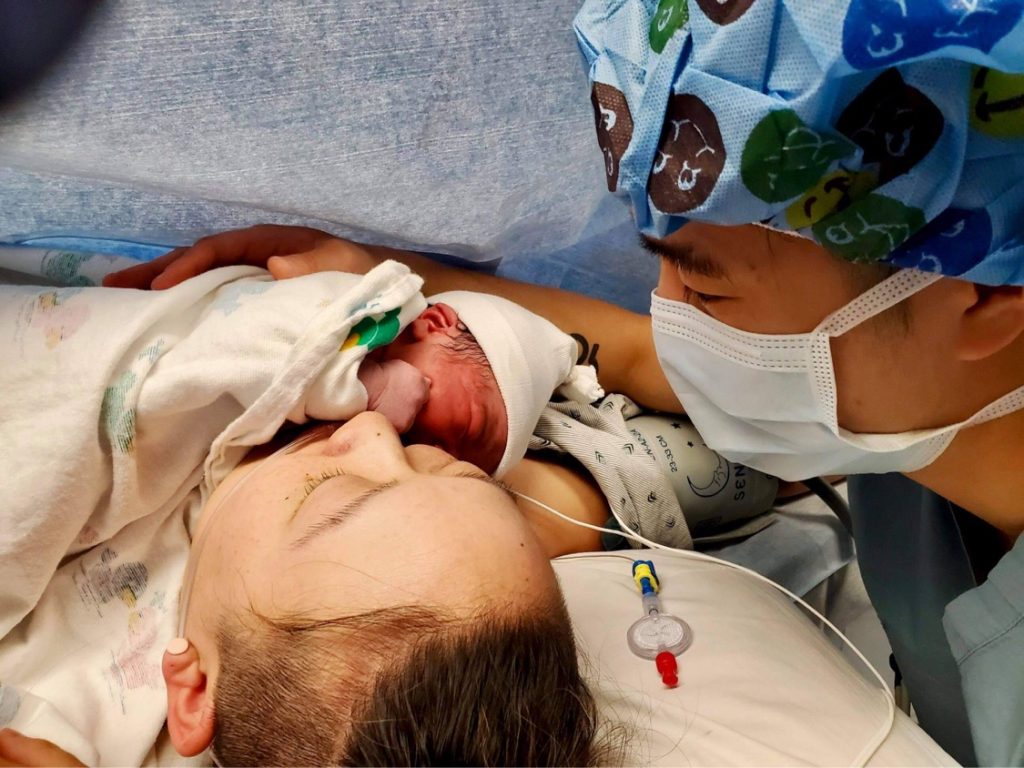
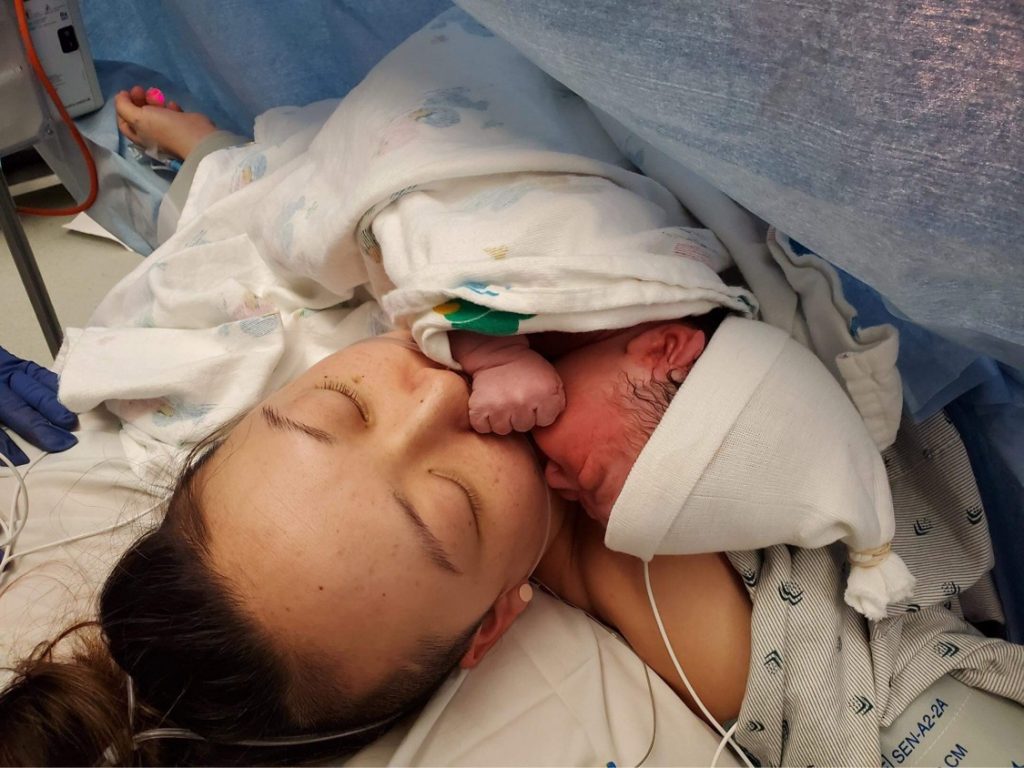
I was able to see JP just after he was born with use of a clear drape. In my birth preferences, I stated that I wanted his cord not to be clamped until it stopped pulsating. Looking at pictures months after, I realized that this wasn’t done. Instead of immediate skin to skin, he was taken to the side for care before being placed near my face. I wish I had asked for my arms not to be restrained during surgery. I was so checked out that I didn’t really think to advocate for myself in the OR, even though prior to labor, I knew that I had all sorts of options, even if I birthed my baby via cesarean.
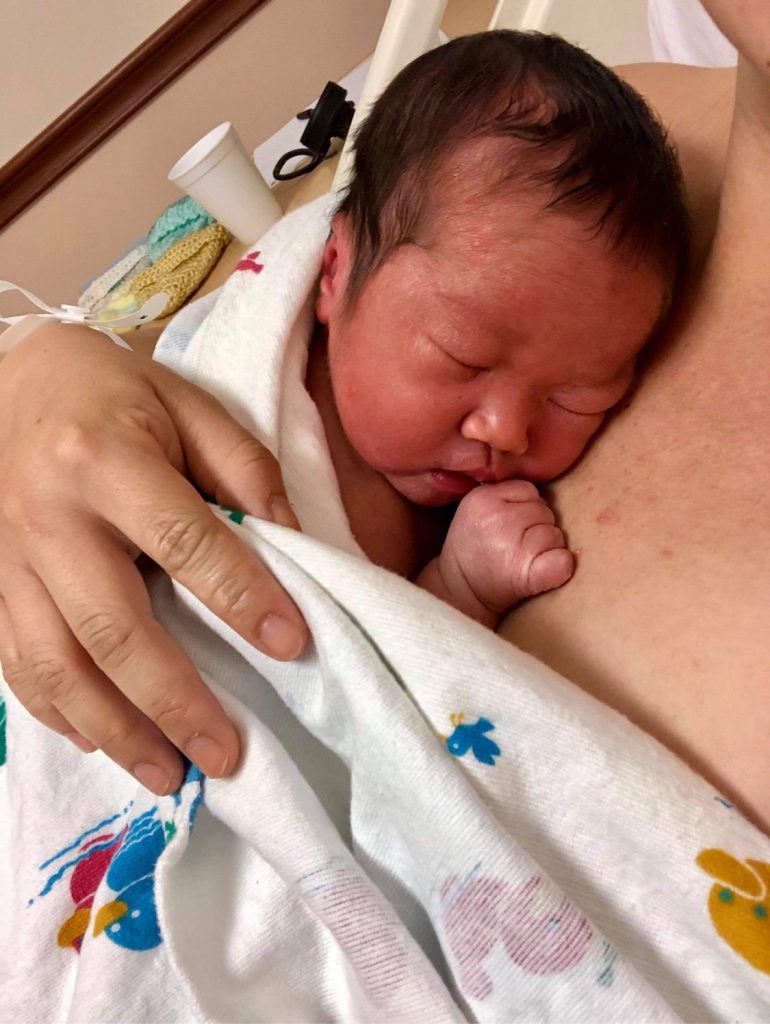
I was able to hold him on our way to recovery and breastfeed once we were in the recovery room. My cesarean recovery went probably as smoothly as it could.
During my baby’s first outpatient pediatrician appointment, the doctor was concerned about jaundice. She recommended that we get his bilirubin checked, which meant we had to go back to the hospital, as outpatient labs were closed for a holiday. She also suggested that we would have to supplement with formula. Driving to the hospital, I felt the same feelings of fear and guilt that I felt before consenting to the cesarean. I blamed myself for missing something and was mad at my body for not providing the nutrition my baby needed.
I wasn’t prepared for the emotions that hit me as I walked through the labor and delivery unit and Birth Place. I sobbed as a nurse held my arm and led us to a private room. She showed us how to feed my breast milk through an open cup, a spoon, and a syringe. Thinking back to these moments, she was such a kind, bright spot in an otherwise difficult time. After a heel stick, she did a quick forehead scan and though his levels were elevated, she thought they were low enough that we might not have to be re-admitted.
Within 5 minutes of arriving back home, we got the call that we needed to go back. I was an emotional mess. I felt tired. And devastated. And guilty.
Shortly after we were re-admitted, the RN seemed to suggest to me that I was putting baby’s health at risk, telling me that I could cause him to have seizures and neurological damage if I didn’t supplement with formula. I was already feeling so vulnerable and it felt like she was thinking I was selfishly making decisions, while I was really just trying to do what I felt was best for my baby. The NP and neonatologist who later came in were happy with the amount of milk I was able to produce and felt comfortable with me supplementing with pumped breast milk. While in the hospital, every 2 hours, we would take him out of the isolette, I would breastfeed for as long as he could tolerate, we would put him back in the isolette under the bili lights, I would pump, and my husband or I would finger feed pumped milk. We would talk, and/or I would cry, and/or we would get a little bit of sleep before repeating the whole process.
For weeks, I would breastfeed and then pump and then my husband would finger/syringe feed what I pumped. We tracked every mL. In the meantime, my baby had a shallow latch that caused intense pain. My husband would do some full finger feedings to help give me a break. I’m a person who has a hard time giving up control. I think preserving breastfeeding was my way of taking back some control after feeling so out of control. I was afraid that introducing a bottle would cause nipple confusion or a bottle preference, but in retrospect, it probably would have been much better for my mental health to have just given some bottles.
Things got better after seeing an IBCLC, though I did experience plugged ducts and mastitis several times.
That birth and those early weeks were the most difficult, rewarding weeks of my life. It wasn’t the start to life I was hoping to give my baby. It wasn’t the peaceful time of recovery and connection I was hoping to have for myself, my baby, and our new little family.
I found out I was pregnant again shortly after our son’s first birthday. I immediately knew that I wanted a homebirth. Now, I’m 33 weeks pregnant. Driving home from my last visit with my midwife, I started thinking about how much love and support will be present in our home when this baby is born. This is what I wanted for my first baby. I still feel guilty that he wasn’t welcomed into the world with the warmth, love, and serenity that I so badly wanted for him. But, I’m so thankful he’s given me the motivation to work through this birth trauma so that I can be the best mom to him and he’ll be able to share in his sister’s birth story.